

You will know Lou Gehrig if you are a baseball fan or a Neurologist. Lou Gehrig whose name has been given to Amyotrophic lateral sclerosis was an "ironman" in baseball unfortunately died of ALS.
Amyotrophic lateral sclerosis is a type of motor neuron disease.
What you need to know in MRCP is that if you get a patient with mixed upper and lower motor neuron with no sensory involvement, you may be dealing with MND. Also if you see fasciculations - MND is high on the list. Of course, don't forget cervical myelopathy and multifocal motor neuropathy with conduction block as differential diagnosis.
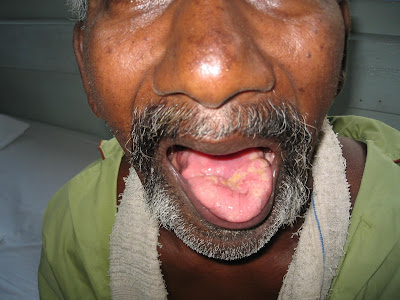
The other possibility in exam is that you are given a patient with bulbar(as in the picture showing fasciculations and wasting of the tongue) or pseudobulbar palsy and one of the underlying aetiology would be MND.
Remember - The lesion is at the anterior horn cell
(first principle of neurology - Where is the lesion ?)




