You will hear this term over and over again from medical school to MRCP PArt 1 to MRCP PArt 2a to PACES(most of the time in history station for differential of headache or transient blurring of vision).
Mean age of diagnosis 70 years old
Slightly more common in women
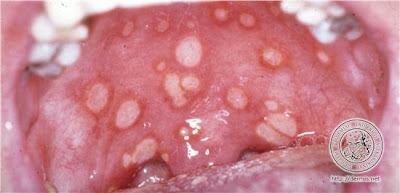
Symptoms :Headache - usually localised
Jaw claudication (pain on chewing)
General malaise
Proximal muscle stiffness and pain
Visual loss (Amaurosis fugax)
Signs :Tender and thickened scalp veins
Optic disc swollen and later pale (AION)
Investigations :ESR elevated (one of the differential for ESR >100)
Raised CRP
Raised ALP
Superficial temporal artery biopsy - intimal thickening and medial damage, giant cells with inflammatory cell infiltration in the internal elastic lamina (GOLD STANDARD)
Management :A general treatment regime for GCA patients that many physicians follow begins with a
70mg/day prednisone dose.
After the first week, the dose is reduced by 10mg every week until the dosage reaches 20mg/day (Schmidt, 2006).
However, some physicians recommend that the high initial dose be maintained for two weeks (Rahman & Rahman, 2005).
Once the 20mg/day level is reached, the dosage is lowered by 2.5mg per week.
Then, when the dosage reaches 10mg/day, it is reduced by 1mg every month depending on the symptoms and test results (Schmidt, 2006).
Most patients remain on corticosteroids for 1-2 years, although some may require long-term steroid treatment (Schmidt, 2006; Piptone
et al., 2005).
The reason that treatment of GCA is usually short in duration is because GCA is a self-limiting disease for most patients (although the mechanism for this limitation is unknown) (Azhar
et al., 2005; Schmidt, 2006).
Longer corticosteroid treatment is typically required for patients with more severe GCA; these patients usually have cytokine levels (such as TNF-α) above most GCA patients (Hernandez-Rodriguez
et al., 2004).
[
www.bio.davidson.edu]

 It's been some while since I last wrote. I have been busy with Neurology. Well, this patient is a 60 years old Malay man who was admitted to my ward with progressive L sided weakness over a week. He is non toxic looking and there is no stigmata of chronic liver disease. He has been a chronic smoker. To tell the truth, I was rather upset that 2 of my house officers could not come to a conclusion even after I mentioned the gross clubbing in this patient.
It's been some while since I last wrote. I have been busy with Neurology. Well, this patient is a 60 years old Malay man who was admitted to my ward with progressive L sided weakness over a week. He is non toxic looking and there is no stigmata of chronic liver disease. He has been a chronic smoker. To tell the truth, I was rather upset that 2 of my house officers could not come to a conclusion even after I mentioned the gross clubbing in this patient.